Are you wondering how to find the best dentist near you? Locating a reliable dentist involves considering several general factors such as accessibility, professional credentials, and patient reviews. It’s important to choose someone who meets your general dental needs and with whom you feel comfortable.
Dentist Near Me: Importance of Local Dental Reviews
When searching for a “dentist near me,” it’s crucial to consider local dental reviews as they provide insights into the experiences of previous patients. These reviews can highlight the strengths and weaknesses of a dental practice, giving you a clearer picture of what to expect. Reviews often cover various aspects, such as the dentist’s communication skills, the efficiency of the staff, and the overall cleanliness of the clinic. By reading through these testimonials, you can gauge the reputation of the dentist in your community and make a more informed decision.
Furthermore, local dental reviews can help you understand how a dentist handles different dental procedures and patient care, which is essential for building trust and comfort. For those interested in specific treatments, such as dental implants, reviews can be particularly valuable. For more detailed information on this topic, consider visiting Indianapolis Dental Implants: A Comprehensive Guide to Restoring Your Smile.
Dentist Near Me: Evaluating Dentist Office Cleanliness
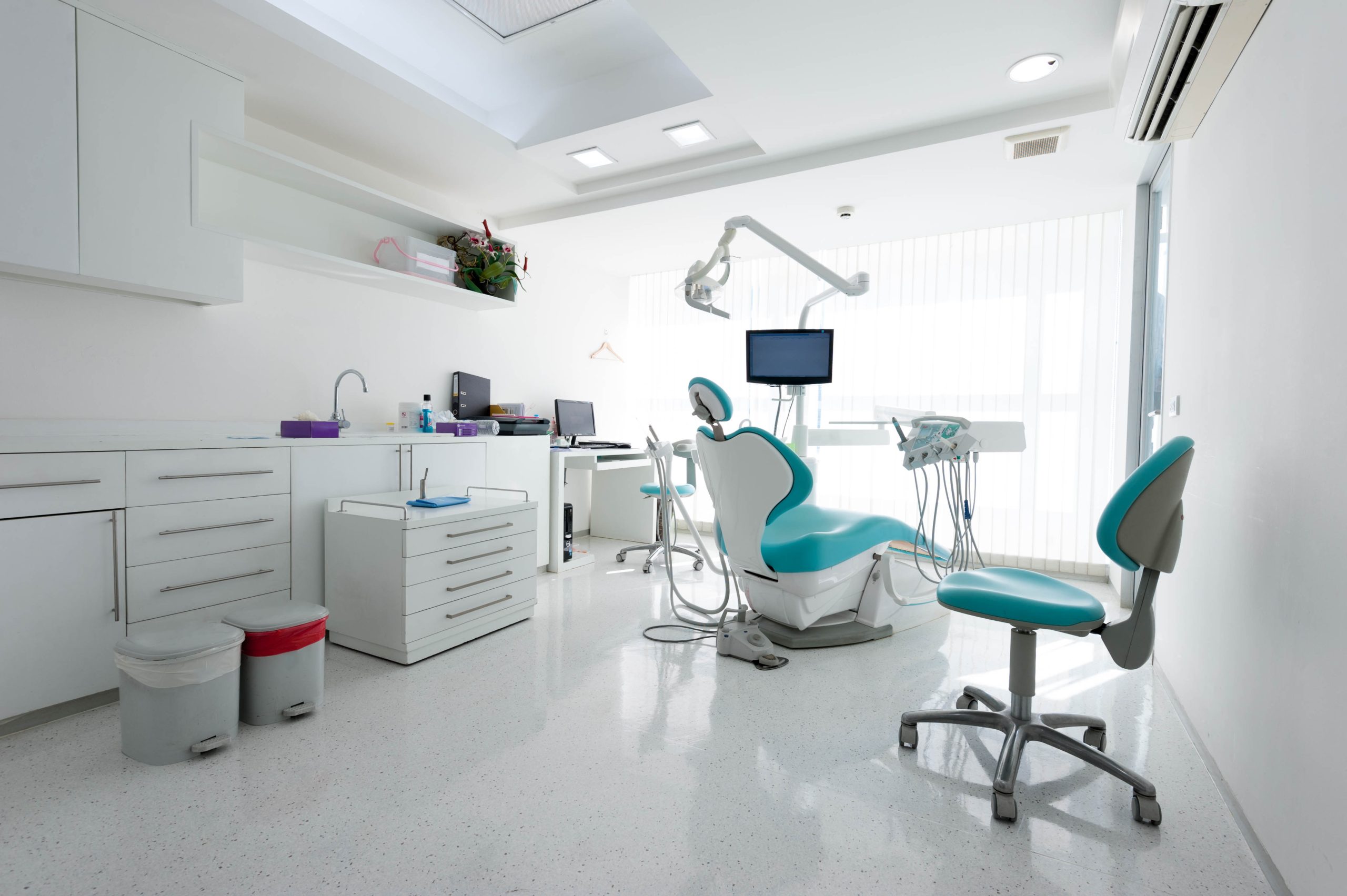
When searching for the best dentist near you, one of the crucial factors to consider is the cleanliness of the dental office. A clean environment not only ensures a hygienic space but also reflects the overall care and attention to detail that the dentist and their staff uphold. Observing the cleanliness of the waiting area, treatment rooms, and even the restroom can give you insights into the practice’s standards. Additionally, noticing whether the dental tools are well-organized and sterilized before use is essential for patient safety and health.
The state of the office often mirrors the quality of services provided. A well-maintained clinic suggests that the dentist values patient comfort and hygiene, which are important aspects of professional dental care. If you’re looking for a reliable and clean dental office, Visit the Best Dentist Near Me in Indianapolis.
Understanding Different Dental Specializations
When searching for the best dentist, it’s crucial to recognize that dentistry encompasses various specializations, each focusing on different aspects of oral health. General dentists provide routine care, preventive measures, and minor restorative therapies. Orthodontists specialize in aligning teeth and jaws, primarily using braces and other corrective appliances.
For gum-related issues, periodontists are the specialists who treat gum diseases and implant procedures. Endodontists focus on root canal therapy and other procedures involving the interior of the tooth. Each specialization addresses specific dental needs, ensuring comprehensive care tailored to individual conditions.
Checking Dentist Credentials and Experience
When searching for the best “dentist near me,” it’s crucial to consider the credentials and experience of the dental professionals. Ensuring that your dentist is properly licensed and has a robust educational background is fundamental. Additionally, reviewing their years of practice and areas of specialization can provide insight into their expertise and proficiency in handling various dental concerns. For those in the Nora area, Indianapolis Dentist at Thompson Family Dental is an example of a practice where verifying credentials can be a starting point.
Importance of Modern Dental Equipment
When searching for the best “dentist near me,” it’s crucial to consider the technology and equipment they use. Modern dental equipment plays a pivotal role in ensuring accurate diagnoses, efficient treatments, and overall patient comfort. Advanced tools such as digital X-rays, laser dentistry, and CAD/CAM technology not only enhance the precision of dental procedures but also significantly reduce recovery times. A dentist equipped with the latest technology is likely to provide superior care, making your search for a top-notch dentist near me both effective and reassuring.
Considering Office Hours and Location
When searching for the best “dentist near me,” it’s crucial to consider both office hours and location. A conveniently located dentist can significantly reduce travel time and stress, especially in case of emergencies. Additionally, dentists with flexible office hours can accommodate your schedule, ensuring you can get dental care without disrupting your daily routine. Make sure the dental office is accessible from your home or work and check if they offer early morning, evening, or weekend appointments to suit your lifestyle.
Assessing Staff Friendliness and Professionalism
When searching for the best “dentist near me,” it’s crucial to consider the importance of modern dental equipment in their practice. Advanced technology not only enhances the accuracy of diagnoses and treatments but also significantly improves your comfort and the efficiency of your dental visits. A dentist who invests in contemporary tools and stays updated with the latest advancements in dental technology demonstrates a commitment to providing top-notch care. This commitment is often reflected in the quality of the results and the overall patient experience, making it a key factor to consider during your search.
Importance of Patient Comfort Measures
When searching for the best “dentist near me,” it’s crucial to consider the importance of patient comfort measures. A good dental practice will prioritize making your visit as comfortable and stress-free as possible. This includes offering a calming environment, gentle treatment methods, and clear communication about procedures.
Dentists who invest in modern amenities such as comfortable seating, soothing music, and pain-free technologies show a commitment to patient care, which can significantly enhance your overall experience. Choosing a dentist who values patient comfort can transform a routine dental check-up into a positive, reassuring encounter.
Recognizing Efficient Dental Practice Management
When searching for the best “dentist near me,” it’s crucial to consider how well a dental office is managed. Efficient dental practice management often translates to shorter wait times, more organized appointments, and overall better patient care. Look for signs such as a clean and organized reception, friendly and responsive staff, and clear communication about services and fees. A well-managed practice will not only ensure that your dental needs are met professionally but also provide a comfortable and stress-free experience during each visit.
Conclusion
For further information, feel free to call us at 317-846-9444 or read our reviews on Google Maps.